How can we use a falls framework to improve the ambulance service response to falls An interview with Claire Roche (Assistant Director for Quality, Governance and Assurance) Welsh Ambulance Service
Originally published by Ian Baines – 17th May 2019
The #ProjectA programme of work has been engaging frontline ambulance staff, colleagues and patients in developing ideas for improvement for the ambulance service. Since late 2018, #ProjectA has been working on a number of improvement themes suggested by frontline staff.
From this we found that a recurring theme was improving the ambulance service response to falls. There was a clear frustration about not always providing the best care and indeed recent estimates highlighted that there are more than 70,000 hip fractures in a year. In addition, falls have been the leading cause of accidental death in older people.
On the 28th January 2019 #ProjectA brought together a number of critical friends and representatives from every ambulance service in the UK to discuss how potential improvements in the ambulance services response to falls could be enacted. You can read the report of the event, and there’s also a blog post that explains more.
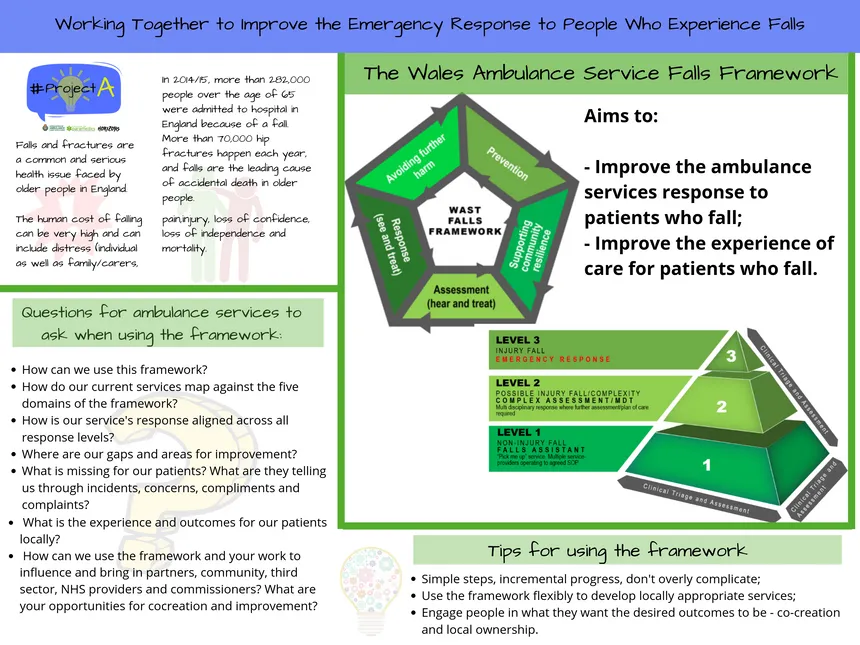
The Welsh ambulance service shared the approach they had taken in designing a Falls Framework and Response category for their fall services. This Falls Framework was identified to be a helpful tool for other ambulance services to understand and improve their own responses. It was determined from this that #ProjectA should look to support the scale and spread of the framework to other ambulance services in the UK.
In looking at how the framework could be used, Ian Baines (NHS Horizons) interviewed Claire Roche (Assistant Director for Quality, Governance and Assurance – Welsh Ambulance Service). Claire had been instrumental in developing the framework in Wales and engaging colleagues in its use and subsequent service improvement
Why did you see the need to develop a falls framework for the Welsh Ambulance service?
We could see by our complaints and incident data that falls, particularly of the elderly, were becoming a frequent occurrence and it got us focused into thinking more and more that we must do something, not only in terms of treatment put prevention also.
We also have a very wide geographical patch, with different social determinants and whilst we knew we had pockets of good practice, understanding the different services, or lack of services, out there had to be a starting point. Did we have gaps and could we bring in learning and investment? In addition we also recognised that how different stakeholders talked about services was often at odds and perhaps didn’t align around the same terminology and expectations. Putting it simply – we needed some clarity over our large patch in relation to our falls services.
Once you had developed the model – how did you use it?
I was going along to our falls steering group and as I mentioned (above) could see that often we were not joined up or talking about services and their improvement in the same manner. At times the steering group was just confused and hard going for all participants. We all had different thoughts and ideas about what we had in place already, where we needed to go and the different stakeholders involved also struggled with how the different services pieced together. We knew we had to untangle this in order to give us something that we all understood in talking about falls and that we could use to categorise our services. It was a long road but eventually we worked through this and the framework started to emerge.
The framework helped us make sense of the broad picture – what is our core business, do we have gaps and are there opportunities in our services to link or do something different? It is a sense making tool that allowed us to start having the coherent conversations around how we could improve or make changes. It focused minds and transformed our mindset so that we could begin to describe our falls services and how they operated. It started to crystallise good conversations with stakeholders and commissioners.
Where have you seen its impact?
Even within a single ambulance service – there will be significant variation in how services are delivered. It is important therefore to acknowledge that you will have variation across your patch and thus in approaching any improvement it is probably best tackled in bite sized chunks. Can you identify a priority? Can you link a gap to complaints? Where can you have an impact? Where is the will and the energy to try something different?
Level 1 response is probably the most logical place to start for most ambulance services as there may be flexible and local solutions that can be employed. For example in one patch we have used the falls framework to have discussions with commissioners about a more appropriate level 1 response – this is now being undertaken by seven St. John’s Ambulance Service ambulances. We are moving now to assessing the impact of this scheme to see if it can be scaled to other areas but are hearted by the early data. We estimate that between October and February St John’s responded to 1,200 incidents that required their support, in an average response time of 55 minutes. Only 29% of these were subsequently conveyed to hospital. In the past these responses were handled by our own ambulances.
Another example is that we have agreed with emergency commissioners to purchase lifting aids for 300 care homes and the associated training. Whilst the framework was still being developed as the discussions were underway, it still helped us clarify our need and the right conversation to have. We have also started to join this work up with wider pressure ulcer reduction work.
Where are you now with the framework?
As we have gained clarity on our services, response and discussions with stakeholders we’ve noted that our steering group has matured with the potential for individual stakeholders to respond to the different levels of the framework and response model. The potential is now there for other stakeholders (be they internal and external) to take on areas of work in falls with confidence and ‘shift’ the steering group onto more of a programme board, co-ordinating the improvement work.
We’ve also linked into the National Falls Task force and we see the wider opportunity of falls within an overall approach to frailty and older people’s plan for the Welsh Ambulance service. Linking and connecting to ongoing frailty work has to be where we go next from a strategic level and we want to explore how we approach frailty, building in responses to loneliness and isolation.
What advice would you offer to all the UK ambulance services out there in using the framework?
The framework is simply a guide and a way of organising services and responses into common themes and language. It is a starting point that allows the thoughts and the conversations to then flow in a more ordered manner. I would say once services and responses have been mapped to the framework – don’t try and bite off too much. Find an area that you know requires an improvement and where there may be opportunity to improve or fill a gap. It takes time – small steps and bite sized chunks have underpinned our progress in Wales.

I would say once services and responses have been mapped to the framework – don’t try and bite off too much. Find an area that you know requires and improvement and where there may be opportunity to improve or fill a gap. Claire Roche
